
Health insurance policies can be complex due to the wide range of medical treatments, procedures, and services that may be covered or excluded under the policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More.
An insurance claim is a formal request made by the policyholderA policyholder is an individual or entity that owns an insurance policy and pays the premium in exchange for coverage. More to an insurance company for cover or compensation for a covered loss. At the beginning of the contract, the insurer charges an insurance premium and promises to pay the amount as per the insurance contract. The insurance company reviews the documentation and determines the amount of coverage that will be provided based on the terms of the policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More and the extent of the loss.
Claim payment is the moment of truth for any customer who buys an insurance policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More. Such moments often result in a polarisation of their opinions about insurance benefits. If the claim is rejected or partially covered, it can lead to dissatisfaction among customers. The other situation can include trust and happy customers, if the claim is fully covered.
To ensure that there are no surprises in insurance at the time of claims, customers should follow some easy steps:
- Know your policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More terms and conditions
- Know the claim intimation and submission timelines
- Know the process of filing a claim
How does a health insurance claim work?
Many people think that the process of health insurance claims is complicated. However, it’s straightforward when you break it down. For example, suppose you visit the hospital for either admission or for a domiciliary stay. In that case, the doctor forwards the prescription to the hospital’s administrative staff. From there, the bill is sent to the insurance company, and the claims processor or the TPA will check it by investigating the accuracy and whether the service is covered under the insured plan.
How are claims settled under health insurance?

The claims settlement process is one of the most important aspects of an insurance policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More, especially if it is a health cover. This is because it is all about the health of an individual.
Policyholders’ health insurance claims can get settled by an insurer through
- Third-party administrators (TPA)
- Through the insurer’s in-house claims processing department.
Third-Party Administrators (TPAs) are independent companies that handle the claims processing and other administrative functions for health insurance companies. They are responsible for reviewing and processing claims, determining coverage, and paying providers for the medical services that are covered under a policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More.
Insurers may also have their own in-house claims processing department to handle claims. In this case, the claims are reviewed and processed by employees of the insurance company rather than an external TPA.
Is a health insurance claim form a bill?
A health insurance claim form is a document used for submitting the claim. By filling this form, the insured can turn to the insurance company for payment as the insurer has promised to cover the insured at the time of need.
What are the four stages of the life cycle of an insurance claim?
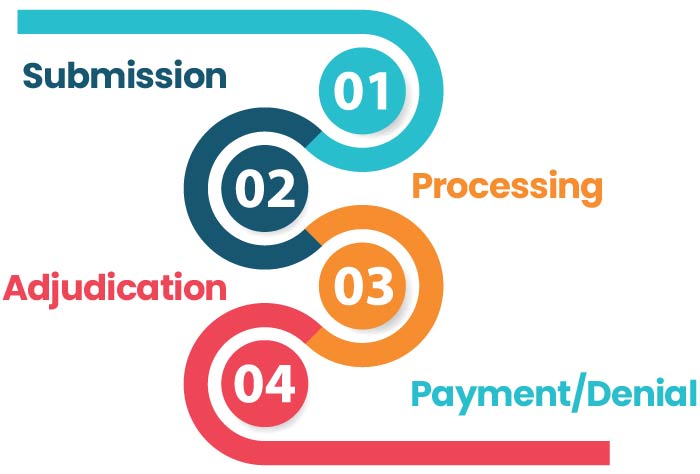
The process of filing an insurance claim can seem daunting, especially if you are unfamiliar with the terminology and procedures involved. One important aspect to understand is the life cycle of an insurance claim, which consists of four stages.
- Submission
The first stage is submission. This is when the insured individual or the healthcare provider submits the claim to the insurance company. The claim typically includes information such as the patient’s name, policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More number, and details of the medical services provided. The claim may be submitted either electronically or through paper forms.
- Processing
Once the insurance company receives the claim, it will begin processing it. This involves verifying the information provided and determining whether the services received are covered under the policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More. The insurance company may also request additional information or documentation to support the claim.
- Adjudication
After the claim has been processed, it will be adjudicated. This means that the insurance company will make a decision about whether to approve or deny the claim. If the claim is approved, the insurance company will determine the amount of coverage that will be provided based on the terms of the policyAn insurance policy is a legally binding contract between an insurance company (insurer) and an individual or business (policyholder). It More and the extent of the loss. If the claim is denied, the insured individual will typically receive a letter explaining the reason for the denial.
- Payment/denial
The final stage of the life cycle of an insurance claim is payment or denial. If the claim is approved, the insurance company will issue payment to the healthcare provider for the services rendered. If the claim is denied, the insured individual will not receive any payment, and they may need to explore alternative options for covering the cost of the services.
Insured individuals should stay informed about the status of their claims and follow up with their healthcare providers and insurance companies as needed. Understanding the four stages of the life cycle of an insurance claim can help make the process less confusing and more manageable.
